Millersburg Spine Specialists Near You
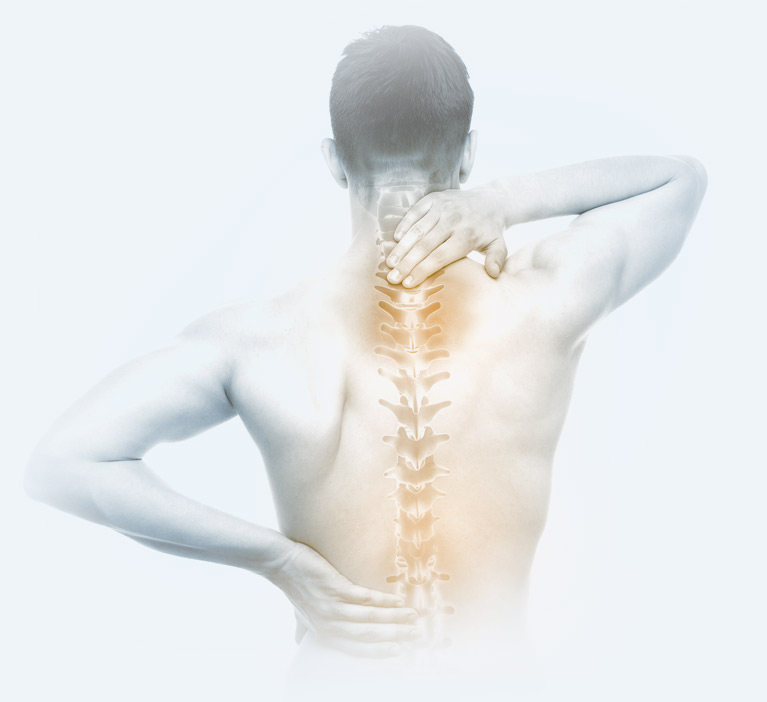
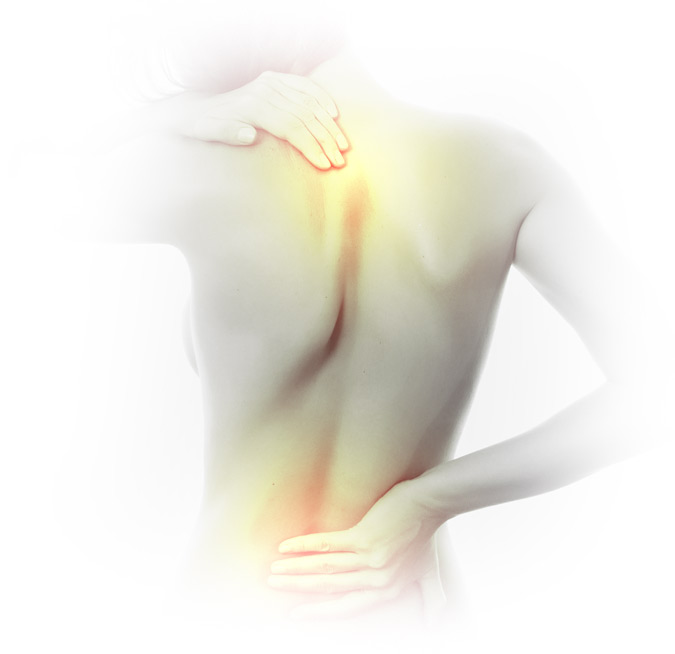
The Orthopedic Institute of PA proudly serves the Millersburg community and beyond by providing advanced orthopedic care to anyone in need. Our commitment to personalized care and improved quality of life sets us apart as the choice for referrals throughout the area. If you experience neck or back pain for more than two weeks or the pain limits your mobility, let OIP’s trusted professionals be your orthopedic pain specialists today.
4.9 stars 4.95 out of 5 (1611 reviews) About star rating